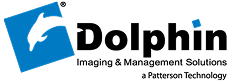Never Call Insurance Again.*
A dedicated team that runs your eligibility checks, benefit breakdowns, portal lookups, and insurer phone calls — with typical turnaround of 24–48 hours before each appointment and a 99%+ completion rate.† Built for Dentrix, Eaglesoft, Open Dental, and other major dental practice management systems.
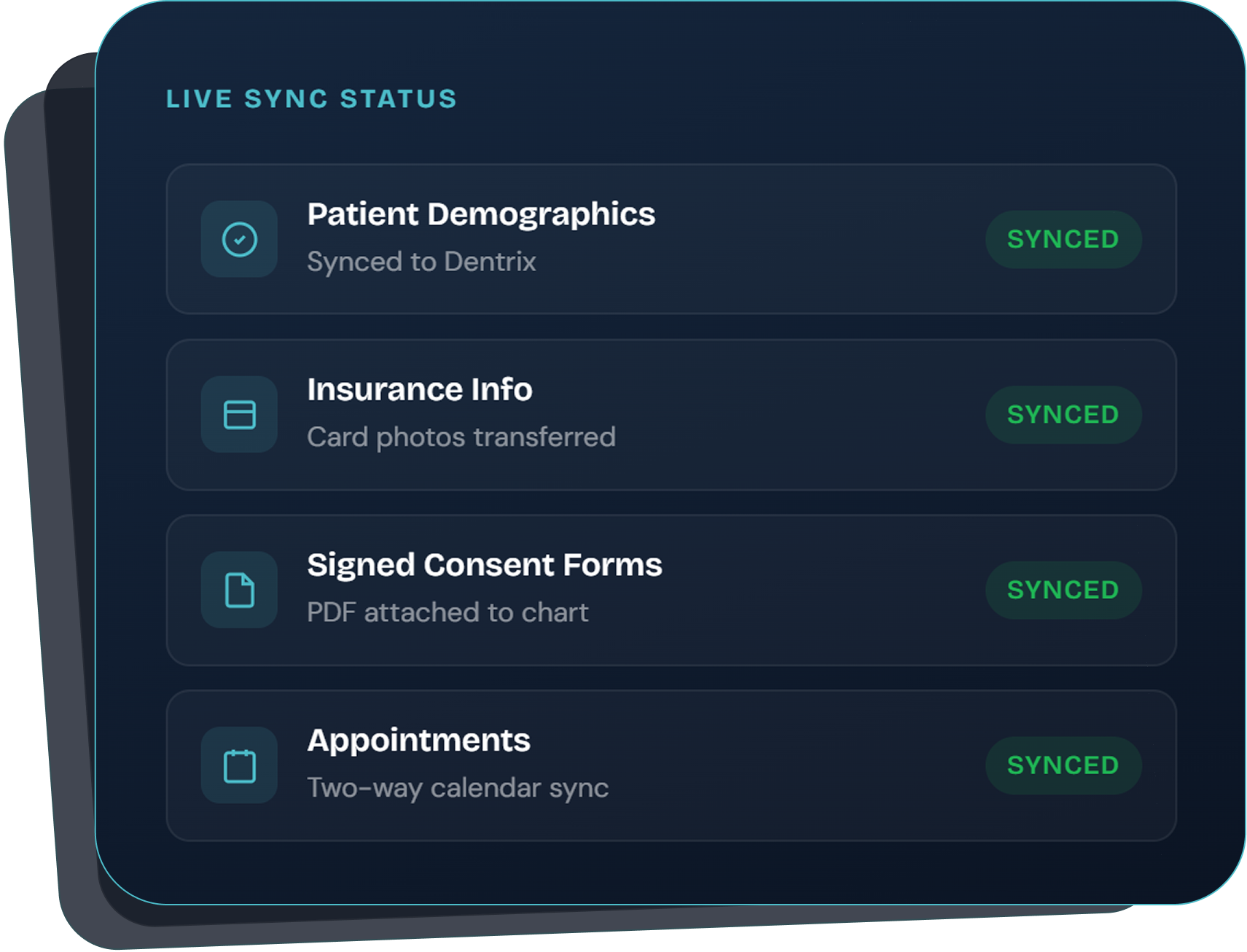
Dental insurance verification can drain your front desk
Industry research suggests 15–25% of claim denials relate to faulty or missing verification, and verification tasks can consume several hours per day of staff time. Insurance Concierge was built to address these challenges.Source: industry surveys and reporting on dental billing; individual practice experience varies.
Short-staffed
Difficulty finding or affording dedicated insurance staff. Existing team stretched thin.
Hours on hold
Staff time spent calling insurance companies and waiting on hold often runs into hours each day.
Claim denials
Errors in manual verification can lead to rejected claims, rework, and lost revenue.
Patient surprises
Patients who discover coverage gaps at checkout can lose trust and satisfaction in your practice.
A dedicated verification team — not just software
We assign a dedicated team of experienced insurance verification agents to your practice, backed by white-glove onboarding and a named account manager. Agents work under a US-based Director of Insurance Concierge.
White-glove onboarding
You're paired with a dedicated account manager who leads onboarding, configures workflows to match your practice, and stays with you post-launch as a single point of contact for questions and escalations.*
We integrate with your PMS
API installation connects us to your practice management system — Dentrix, Eaglesoft, Open Dental, Dolphin, Athena, Dentrix Ascend, OfficeMate, PBS Endo, or other major dental PMS environments. Google Chat provides your team a direct line to our agents.
We verify in advance
Our agents complete eligibility checks and benefit breakdowns typically 24–48 hours before each appointment,† using insurer portals, phone calls, and fax-backs. Full dental breakdowns are uploaded directly to your PMS — no rekeying.
Your team focuses on patients
Verified breakdowns are available in your PMS ahead of the patient visit. Designed to reduce time on hold and claim denials from missing verification data — with your account manager monitoring success throughout.
*Specific onboarding scope, implementation timelines, go-live dates, and ongoing account management terms are defined in your Master Service Agreement with mConsent. Verification outcomes depend on accurate data from patient insurance portals, which mConsent does not control.
Your own dental insurance verification team
This isn't a chatbot or automated-only tool — it's a managed team of experienced insurance verification agents, led by a US-based Director of Insurance Concierge. The team adopts your workflows and scales with your practice.
- Dedicated account manager — a named point of contact who leads white-glove onboarding and stays involved post-launch.
- US-based Director — the Director of Insurance Concierge is US-based and leads the program.
- Experienced agents — trained in dental insurance with portal knowledge.
- Continuous coverage — designed to reduce coverage gaps when your team is unavailable.
- Dedicated Google Chat channel per practice — a 1-on-1 line to your IC team for real-time questions, flags, and instant alerts on inactive or terminated policies.
Team composition includes US-based leadership and trained offshore verification agents who operate under HIPAA Business Associate terms. All PHI handling follows the safeguards described in our security practices.
Four ways to verify insurance. One that actually works.
Most practices try verification software, remote agencies, or a full-time coordinator before landing on Insurance Concierge. Here's how the four approaches stack up.§
§Completion-rate ranges for Verification Software, Remote Agencies, and Insurance Coordinator reflect general industry observations on dental verification workflows and published dental revenue cycle research. These are broad industry ranges and do not represent the results of any specific competitor. †mConsent Insurance Concierge completion rate based on mConsent system logs; individual practice results vary with insurer portal availability and patient data accuracy. ‡Pricing is tailored to verification volume and complexity. Plan tier and specific inclusions are defined in your Master Service Agreement. See FAQ for starting-price details.
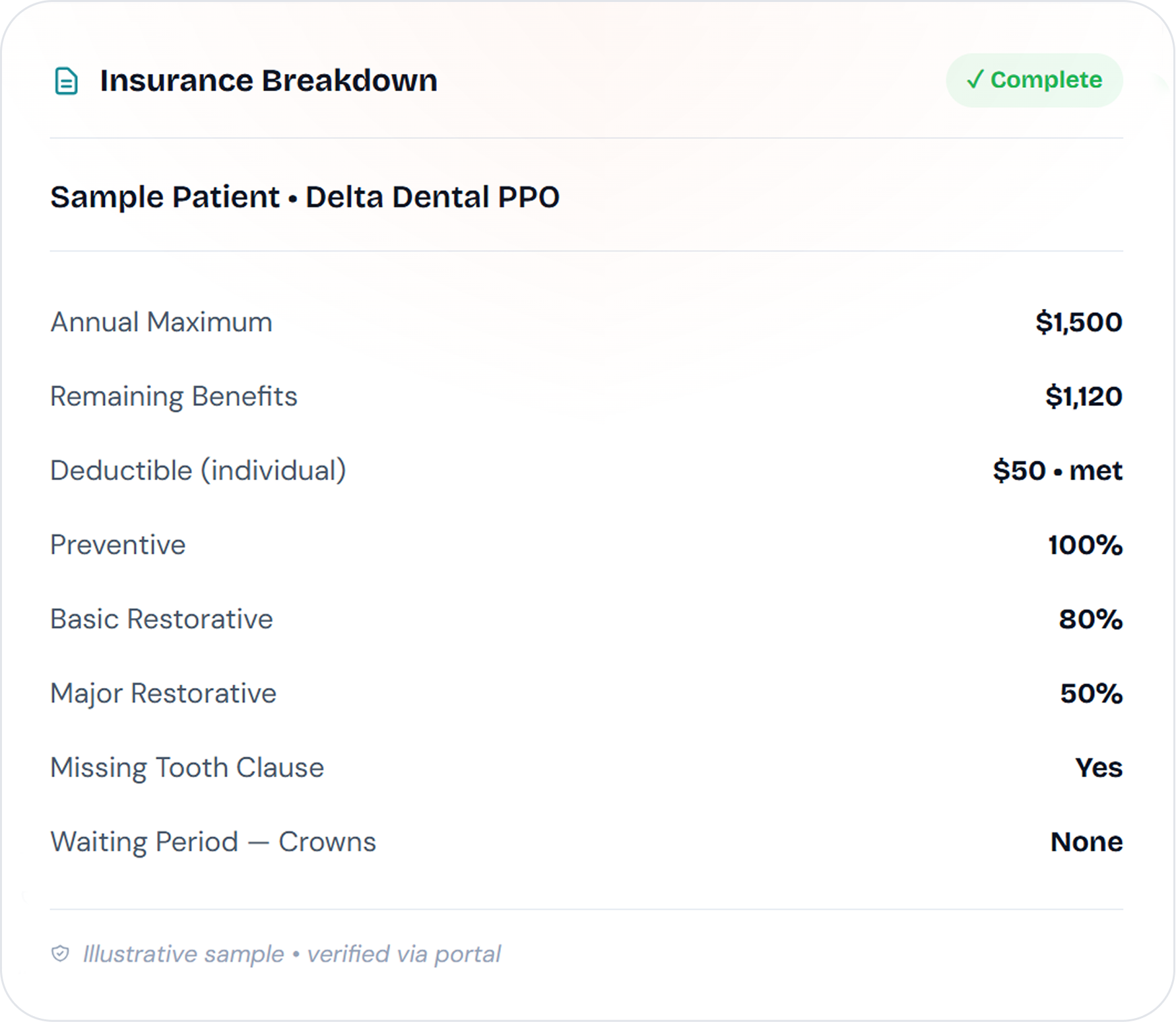
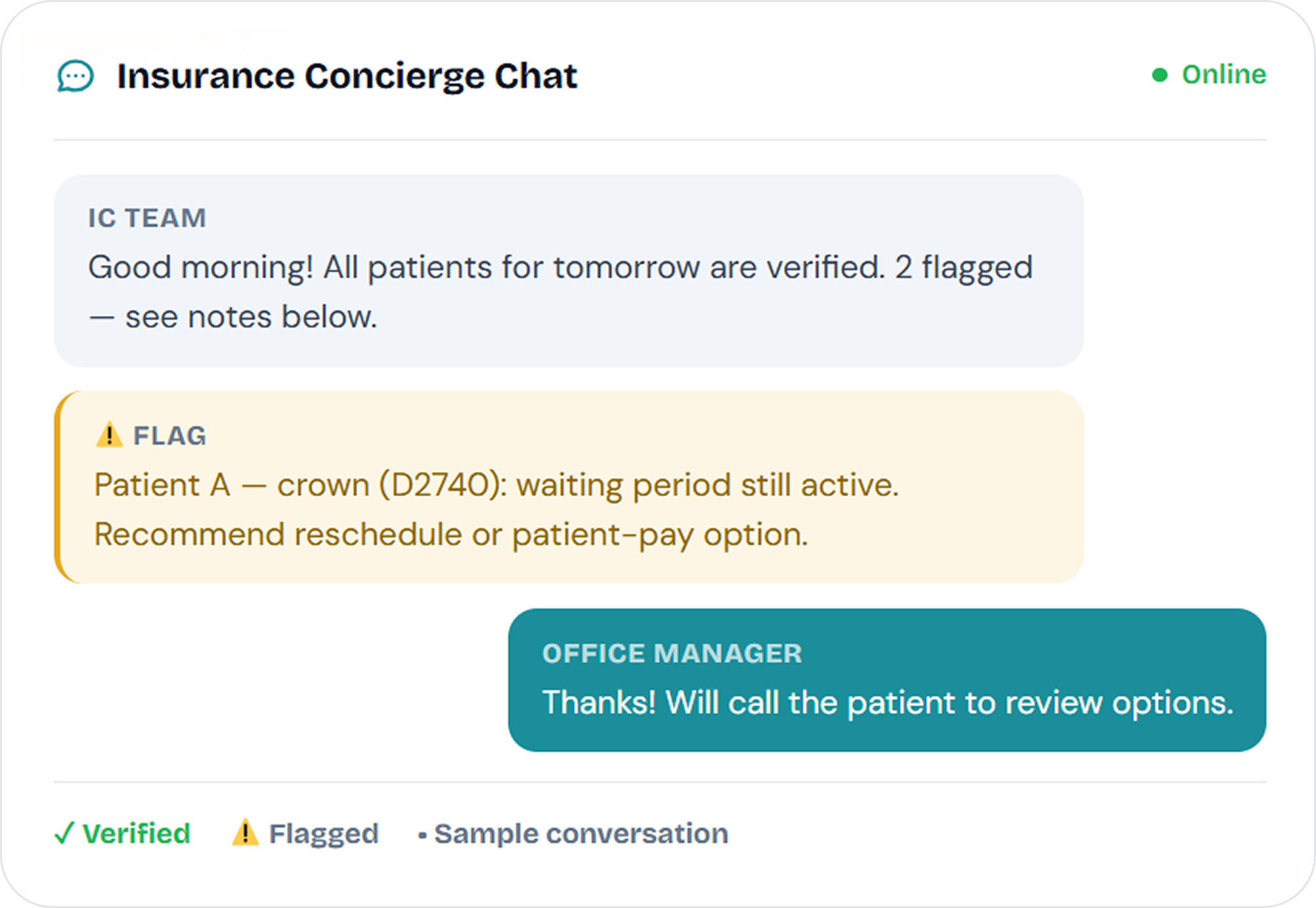
Detailed dental insurance breakdowns
We don't just check eligibility — we aim to provide full dental breakdowns tailored to your office's needs. Maximums, deductibles, fee schedules, waiting periods, coverage tables, missing tooth clauses, and eligibility by procedure code.
- Secondary & family insurance — we verify all policies, not just primary.
- Re-verification — when plans change, re-verifications are handled by the team as quickly as portal access allows.
- Uploaded to your PMS — breakdowns posted directly to patient records.
What's included in every breakdown
Our agents verify and document the fields your practice needs. Actual fields captured can be tailored to your specific workflow.
Insurance Concierge helps your entire team
White-glove onboarding & success*
A dedicated account manager leads onboarding, tailors workflows to your practice, and stays engaged post-launch to support your team's success. Implementation timelines are defined in your Master Service Agreement.
Clarity & no training burden
Visibility into verification status through reports and Google Chat. No need to create training materials or manage the verification process internally.
One less major task
Designed to reduce time spent on hold. Access to training resources. Collaboration with the IC team via Google Chat. More focus on patients in the chair.
Fewer surprises
Insurance details reviewed before the appointment — designed to reduce unexpected costs at checkout, subject to accurate data from the patient's insurer.
Software, tools & training — bundled
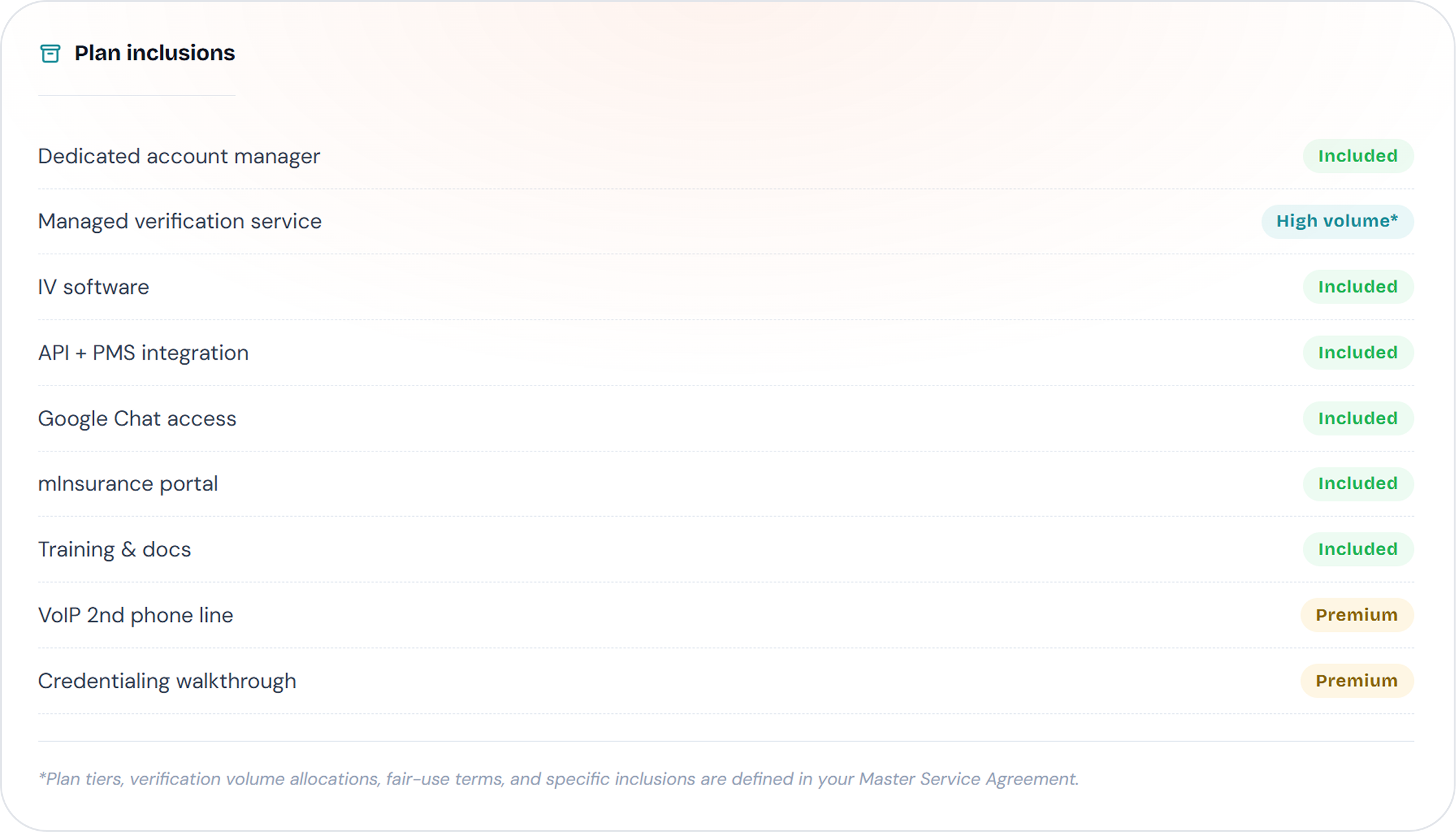
Insurance Concierge is designed to include everything your practice needs to go live. Specific inclusions and plan details are defined in your Master Service Agreement.
- Dedicated account manager — white-glove onboarding and ongoing success partner.
- API integration — connection to your EMR/PMS.
- mConsent IV software — included with Insurance Concierge plans.
- mInsurance web portal — access verified breakdowns from any browser.
- Google Chat access — direct communication with your IC team.
- Document center — process walkthroughs, breakdown templates, training materials.
- VoIP phone line — a second line for agent calls to insurers (Premium plan).
Managing insurance for 60 patients a day was overwhelming, but mConsent helped free the team from time-consuming verification and errors, making the workflow smoother and happier.
Individual practice experience. Testimonials are not typical; results vary by practice size, patient volume, payer mix, and other factors. See disclosures below.
Dental insurance verification FAQs
What is mConsent Insurance Concierge?
What does dental insurance verification include?
How fast are eligibility checks and benefit breakdowns?
Does Insurance Concierge help reduce claim denials?
Which practice management systems does Insurance Concierge support?
Who is on the Insurance Concierge team?
Is Insurance Concierge HIPAA compliant?
How is this different from insurance verification software?
What does onboarding look like?
How is Insurance Concierge priced?
Request Your Free Insurance Audit
See how much time your front desk could save. A dedicated team, typical 24–48 hour turnaround,† full dental breakdowns uploaded to your PMS, and a direct Google Chat line to your IC team — designed to take verification off your front desk.
Important disclosures & fine print
Verification outcomes depend on insurer portals, patient-provided data, and other factors outside mConsent's control — so claim denials, turnaround times, and completion rates vary by practice. Figures, comparisons, and testimonials on this page are illustrative; your specific plan tiers, pricing, and service terms are set in your Master Service Agreement. mConsent operates as a Business Associate under HIPAA and executes a BAA with each customer.
"Never Call Insurance Again" headline. "Never Call Insurance Again" refers to the verification workflow that Insurance Concierge is designed to remove from your front desk. Insurance Concierge is designed to take routine eligibility checks, portal lookups, and insurer phone calls off your team; some complex cases, patient disputes, and clinical-documentation follow-ups may still require direct involvement by your practice. Verification results depend on the accuracy and responsiveness of insurer portals, insurer phone systems, and patient-provided insurance information, which mConsent does not control.
Turnaround times. "Typically 24–48 hours" reflects observed turnaround across Insurance Concierge verifications based on mConsent system logs. Actual turnaround on any individual verification varies with insurer portal availability, phone-system hold times, complexity of the plan, and accuracy of patient-provided insurance information. "Typical" is not a contractual service-level commitment; specific performance expectations and remedies (if any) are defined in your Master Service Agreement.
Comparison table sources & methodology. Completion-rate ranges shown for "Verification Software" (30–60%), "Remote Agencies" (80–95%), and "Insurance Coordinator" (95–99%) reflect general industry observations and published dental revenue-cycle research on verification workflow performance. These ranges are illustrative, are not measurements of any specific named competitor, and are not intended as endorsements or disparagements of any specific vendor. Typical monthly cost figures ($90–120 for verification software, $2,000+ for remote agencies, $4,000+ fully loaded for an in-house coordinator) are representative market figures based on publicly available pricing data and staffing cost benchmarks; actual costs vary by vendor, scope, and geographic market. The 99%+ completion rate for mConsent Insurance Concierge is based on mConsent system logs; individual practice results vary.
Pricing, plan tiers & Master Service Agreement. Insurance Concierge is priced on a per-verification basis. Final pricing for your practice is set in your Master Service Agreement and scales with verification volume, plan complexity, custom workflow requirements, and any add-on services. Plan tiers, verification volume allocations, fair-use terms, and specific inclusions are defined in your MSA. Contact mConsent sales for a quote sized to your patient volume and payer mix.
Testimonials & individual results. Testimonials on this page describe individual customer experiences and are not typical. Individual results are not guaranteed and vary by practice size, patient volume, payer mix, workflow, insurer responsiveness, clinical documentation, coding accuracy, and many other factors.
Team composition. Insurance Concierge is led by a US-based Director of Insurance Concierge. Verification agents include trained offshore team members who operate under HIPAA Business Associate terms and follow mConsent's administrative, physical, and technical safeguards. All PHI is handled under the HIPAA BAA executed with your practice.
Statistics cited on this page. References to "15–25% of claim denials from faulty verification" and hours-per-day spent on insurance calls reflect general industry research and reporting on dental billing workflows. These are broad industry figures, not a measure of denial rates at any specific practice, and individual practice experience varies. Lifetime statistics on this page (5,000+ practices since 2017, 5.5M+ patients served, 30M+ documents processed) are derived from mConsent system logs as of April 2026.
Integrations & trademark notices. "Authorized Dentrix Connected Partner" refers to mConsent's current status in the Dentrix Connected program operated by Henry Schein One. "Dentrix" and "Dentrix Ascend" are trademarks of Henry Schein One. "Eaglesoft" is a trademark of Patterson Dental Supply, Inc. "Open Dental" is a trademark of Open Dental Software, Inc. "Dolphin" is a trademark of Patterson Dental Supply, Inc. Use of these marks on this page identifies the dental practice management systems that Insurance Concierge integrates with and does not imply endorsement, affiliation, or sponsorship beyond the integration relationships disclosed.
HIPAA & Business Associate Agreement. mConsent operates as a Business Associate under HIPAA and executes a Business Associate Agreement (BAA) with each customer. Insurance Concierge team members handle PHI under the same administrative, physical, and technical safeguards that apply across mConsent. View our security practices →
Service boundary notice. Insurance Concierge is a managed verification service. Patients are ultimately responsible for understanding their own insurance coverage; coverage decisions and claim adjudication are made by insurers, not by mConsent.